Prescription of medicines for the management of childhood acute watery diarrhoea at a tertiary hospital in Ebonyi state, Nigeria
Keywords:
Acute watery diarrhoea, Under-fives, Prescriptions, MedicinesAbstract
Background: The burden of childhood diarrhoea in Nigeria is huge and has been persistently high over the years with an estimated 205 under-fifives dying daily. Asimple combination of oral rehydration salts (ORS) and zinc tablets (ORS/Zinc) has been approved for its treatment by the WHO since it is benefificial for rehydration which is the goal of therapy. However, huge resources are spent on antibiotics and other medications which are not benefificial for rehydration, thereby exposing children to unnecessary medications and other drug therapy problems. This study was set to evaluate the prescription of medicines for acute watery diarrhea (AWD) in under-fifive children and to determine the appropriateness of these prescriptions.
Method: This study was conducted in a tertiary hospital in Abakaliki, Ebonyi State. It was a retrospective review of prescriptions of medicines for AWD in under-fifives for a period of 28 months (January 2019 to April 2021). All available cases of AWD (338) were extracted from the prescription registers. Data were entered into SPSS version 24.0 and descriptive analysis was done. The guideline set by WHO for the management of AWD was followed for evaluating the prescriptions.
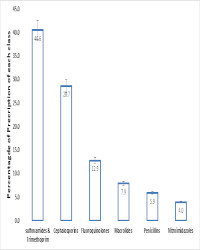
Results: Out of the 338 cases of AWD, 190 (56.2%) occurred in male children and 265 (84.4%) in children under 24 months. Of the total cases, 291 (86.1%) received prescriptions containing ORS, zinc, and probiotics either alone or in difffferent combinations with only 154 (45.6%) containing ORS and zinc together. Of these prescriptions with ORS/Zinc, 47 (30.5%) also contained antibiotics, antimalarials and infusions. In total, there were 99(29.3%) and 48 (14.2%) prescriptions containing antibiotics and antimalarials respectively. The most frequently prescribed antibiotic classes were sulfonamides (41; 40.6%), cephalosporins (29; 28.7%) and flfluoroquinolones (13; 12.9%). Less prescribed antibiotic classes include macrolides, penicillins and nitroimidazoles. Other groups of medicines prescribed were analgesics, anthelmintics, oral potassium and antacids, and antihistamines. Overall, only 107 (36.8%) prescriptions were appropriate for the management of AWD.
Conclusion: This study revealed that only 36.8% of AWD cases received appropriate prescriptions according to guideline. Therefore, there is urgent need for intervention in the study setting to improve appropriate treatment of AWD.
References
International Vaccine Access Center (IVAC), John Hopkins Bloomberg School of Public Health. (2020). Pneumonia and Diarrhoea Progress Report 2020.
Demissie GD, Yeshaw Y, Aleminew W and Akalu Y (2021). Diarrhoea and associated factors among under-five children in sub-Saharan Africa: Evidence from demographic and healthsurveysof34 Sub- Saharan countries .PLoSONE 16(9):e0257522. https://doi.http.org/10.1371/journal.pone.025752
United Nations Children's Fund (UNICEF). (2018). CoD_Diarrhoea_Feb-2018_WHO_MCEE_234. https://www.scribd.com/document/418112664/CoD-Diarrhoea-Feb-2018-WHO-MCEE-234-xlsx
Ofora VC, Ezechukwu CC, Ebenebe JC and Elo-Ilo JC (2020). Economic burden of acute diarrhoea in children aged 6-36 months presenting to a tertiary hospital in southeast, Nigeria. Nigerian Journal of Paediatrics 47(3);227 - 233 doi
https://dx.doi.org/10.4314/njp.v47i3.6
Ogbo PU, Aina BA and Aderemi-Williams RI (2014). Management of Acute Diarrhoea in Children by Community Pharmacists in Lagos, Nigeria. Pharmacy Practice 12(1); 1-6. https://dx.doi.org/10.4321/s1886-36552014000100002.
Carvajal-Vélez L, Amouzou A, Perin J, Maïga A, Tarekegn H, Akinyemi A, Shiferaw S, Young M, Bryce J and Newby H (2016). Diarrhoea Management in Children Under Five in Sub-Saharan Africa: Does the Source of Care Matter? A Countdown Analysis. Bio Med Central Public Health16 (830). https://doi.org/10.1186/s12889-016-3475-1
Obijuru LD, Oyetunde OO and Ogbo PU (2020). Exploration of Barriers to the Recommendation of Oral Rehydration Salts and Zinc Tablets for Acute Diarrhoea by Patient and Proprietary Medicine Vendors in Lagos state, Nigeria. Journal of Basic and Social Pharmacy Research 1(3); 31-40.https://doi.org/10.52968/27451712
Ogbo PU, Soremekun RO and Aina BA (2021). Home management of acute diarrhoea by under-five caregivers in Ikorodu LGA, Lagos Nigeria. West African Journal of Pharmacy 31(1); 151-164.
Ogbo PU, Aina BA and Owoborode OE (2021). The Prescription of Medicines for Childhood Acute Diarrhoea: a Retrospective Study at Four Secondary Healthcare Facilities in Lagos State, Nigeria. Nigerian Journal of Pharmaceutical Research17 (2); 257-265. https://dx.doi.org/10.431/njpr.v17i2.11
World Health Organization (WHO). (2017). Diarrhoeal disease. https://www.who.int/news-room/fact-sheets/detail/diarrhoeal-disease
World Health Organization/United Nations Children's Fund (WHO/UNICEF). (2004). WHO/UNICEF Joint Statement Clinical Management of Acute Diarrhoea
Tsige AG, Nedi Tand Bacha T(2020). Assessment of the Management of Diarrhoea among Children under-five in Addis Ababa, Ethiopia. Pediatric Health, Medicine and Therapeutics 11: 135–143. https://doi:10.2147/PHMT.S243513
Qureshi S, Resham S, Hashmi M, Naveed AB, Haq Z, Ali SA (2021). A retrospective review on antibiotic use in acute watery diarrhoea in children in a tertiary care hospital of Karachi, Pakistan. PLoS ONE 16(7): e0253712. https://doi.org/10.1371/journal.pone.0253712
Okoh BAN and Alex-Hart BA (2014). Home Management of Diarrhoea by Caregivers Presenting at the Diarrhoea Training Unit of a Tertiary Hospital in Southern Nigeria. British Journal of Medicine & Medical Research 4(35); 5524 – 554.
https://doi:10.9734/BJMMR/2014/11340
Raji MO, Abdullahi U, Raji IA Oladigbolu RA, Kaoje AU and Awosan KJ (2017). Caregivers' Knowledge, Home Treatment of Diarrhoea Disease and Predictors of Child Diarrhoea Disease in a Semi urban Community of Sokoto, North-west, Nigeria. Journal of Public Health Epidemiology9: 16–23. https://doi.org/10.5897/JPHE2016.0889
Abdu H, Olusunde Z, Zango A. and Owogbenja M (2013). Assessing the Capacity of Community Health Workers on the Current Management of Childhood Diarrhoea in Jigawa State, Nigeria. Jos Journal of Medicine 7(1); 27 – 31. https://www.ajol.info/index.php/jjm/article/view/89181
Devi G, Rai J, Singh A and Singh K (2015). Prescription Audit for Acute Diarrhoea in Children under five in Tertiary, Secondary and Private Care Hospitals in Amritsar, Punjab. Journal of Evolution of Medical and Dental Sciences4 (50); 8753–8758. https://doi.org/10.14260/jemds/2015/1268
Ogbo PU, Soremekun RO, Oyetunde OO and Aina B A (2019). Prescribing Practices in the Management of Childhood Diarrhoea in Primary Health Care Centers in a Sub-Urban Community in Lagos, Nigeria. Journal of Community Medicine
and Primary Health Care 31(1); 32-39.
Wennberg JE, McPherson K and Goodman D (2015). Small Area Analysis and the Challenge of Practice Variation. Medical Practice Variations, (Issue 1). https://doi.org/10.1007/978-1-4899-7573-7
Akande T. (2004) Referral system in Nigeria: Study of a tertiary health facility. Annals of African Medicine 13(3): 130 – 13. https://doi:10.1149/1.3557879
Aguwa EN, Arinze-Onyia SU, Okeke T and Aniwada EC (2010). Excessive and Inappropriate Utilization of a Tertiary Health Center in South-East Nigeria, TAF Previous Medical Bulletin 9(1); 1 5 – 2 2 . https://catalog.ihsn.og/index.php/citations/61335.
Okoli H, Obembe T, Osungbade K, Adeniji F, and Adewole D (2017). Self-Referral patterns among federal civil servants in Oyo State, South-Western Nigeria. Pan African Medical Journal. 26: 1–11. https://doi:10.11604/pamj.2017.26.105.11483
About Ebonyi State 2022 https://www.Ebonyistate.gov.ng/population.aspx. Accessed on February,13 2022
Abakaliki, Nigeria, Statistics 2022 https://zhujiworld.com/ng/1307766-abakaliki. Accessed on February,13 2022
World Health Organization. (1993). How to investigate drug use in health facilities. http://apps.who.int/medicinedocs/pdf/s2289e/s2289e.pdf
Zhou C, Wang XL, Zhou XD, Hesketh T (2012). Son preference and sex-selective abortion in China: Informing policy options. International Journal of Public Health 57; 459 – 65. https://doi:10.1007/s00038-011-0267-3
Ozumba G. (2005) Gender-sensitivity in Igbo culture: A philosophical re-appraisal. Quodlibet Journal. 7:1–7. IS
Nie JB. (2011) Non-medical sex-selective abortion in China: Ethical and public policy issues in the context of 40 million missing females. British Medical Bulletin 98: 7 – 20. https://doi:10.1093/bmb/ldr015
Ohagwu CC, Eze CU, Odo MC, Abu PO and Ohagwu CI (2014). Perception of Male Gender Preference among Pregnant Igbo Women. Annals of Medical and Health Science Research 4 (2): 173-178, https://doi:10.4103/2141-9248.129027
Platts-Mills JA, Babji S, Bodhidatta L, Gratz J, Haque R, Havt A, Mccormick BJJ, Rayamajhi BB, Qureshi S, Kabir F, Yori PP, Mufamadi B, Amour C, Carreon JD, Richard SA, Lang D, Bessong P, Mduma E, Ahmed T, Lima AAAM, Merson CJ, Zaidi AKM, Bhutta ZA, Kosek M, Guerrant RL, Gottlieb M, Miller M, Kang G, Houpt ER and The MAL-ED Network Investigators (2015). Pathogenspecific burdens of community diarrhoea in developing countries: a multisite birth cohort study
(MAL-ED). Lancet Global Health3: e564-575.https://doi:10.1016/S2214-109X(15)00151-5
Panchal JR, Desai CK, Iyer GS, Patel PP, Dikshit RK. (2013). Prescribing pattern and appropriateness of drug treatment of diarrhoea in hospitalised children at a tertiary care hospital in India. International Journal of Medicine and Public
Health3: 335-41 https://doi:10.4103/2230-8598.123522
Gwimile JJ, Shekalaghe SA, Kapanda GN and Kisanga ER (2012). Antibiotic prescribing practice in management of cough and/ or diarrhoea in Moshi Municipality, Northern Tanzania: cross-sectional descriptive study. Pan African Medical Journal12: 103 http://www.panafrican-med-journal.com/content/article/12/103/full/
Meremikwu A, Udoh E, Esu E, Chibuzor M, Effa E, Oduwole O, Arikpo D and Odey, F (2015). Facility-Based Treatment of Under-five Diarrhoea in Cross River State: A Clinical Audit. Nigerian Journal of Paediatrics 42(4); 314–318. https://dx.doi.org/104314/njp.v42i4.6
Efunshile AM, Ezeanosike O, Nwangwu CC, König B, Jokelainen P and Robertson LJ (2019). Apparent overuse of antibiotics in the management of watery diarrhoea in children in Abakaliki, Nigeria, BMC Infectious Diseases. 19 (1); 1–7.
https://doi.org/10.1186/s12879-019-3899-1
Gadanya, Muktar. (2013). Country Implementation Plan for United Nations Commission on Life-Saving Commodities for Women and Children. https://doi.org/10.13140/RG.2.2.13512.11525
Published
How to Cite
Issue
Section
License

This work is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License.





